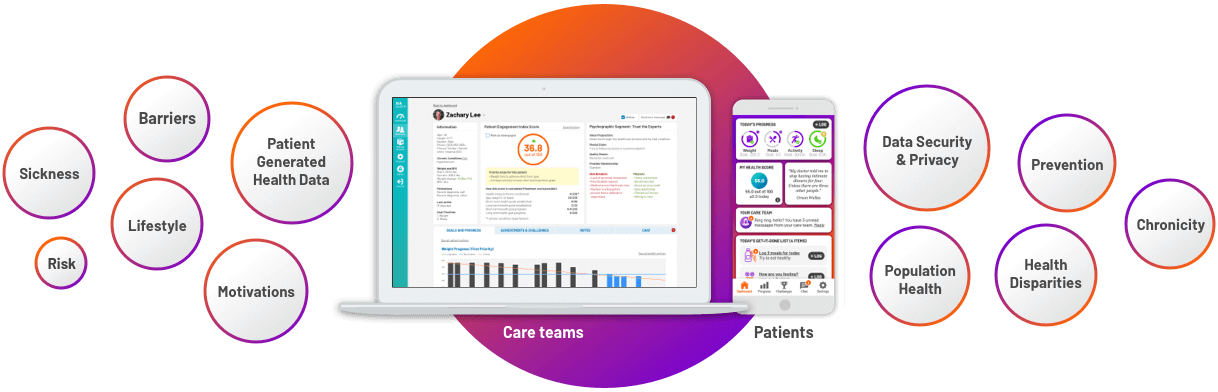
Remote patient monitoring (RPM/RTM) represents an exciting opportunity for providers and practices to improve patient outcomes, lower costs, improve patient satisfaction & engagement, and increase provider revenue. Everyone benefits.
Topics: transforming healthcare, value-based care, remote patient monitoring
Remote Physiologic Monitoring devices provide care teams with both longitudinal and acute data to facilitate intervention at critical points, which leads to the RPM industry’s core metrics of avoidance of hospitalizations or readmissions after an acute episode. These are huge cost drivers, but are those really the targets we should be shooting for? I don’t think so, but existing RPM solutions are not built to deliver more. Ultimately, remote care solutions, including RPM, should first seek to change behavior and lower risk, then seek to intervene in acute episodes as needed. We need to rethink RPM.
RPM should be a component of a larger Remote Care Platform, RCP. Here are our core truths related to this topic.
- Remote monitoring should primarily be embedded in a larger remote care technology platform and strategy. Remote care focuses on patient generated data beyond just device data including diet, exercise/activity, mood, sleep, medication and care plan adherence, etc. The individual’s weight, blood pressure, blood glucose, oxygen saturation, and/or lung function data from the RPM device is then contextualized to the modifiable risk factor data supporting patient behavior change and opening the door for clinicians to get at root cause behaviors. With remote care, behavior change is a critical factor.
- Remote care platforms should drive/facilitate efficient and effective interaction between the care team and the patient. RPM solutions today are almost exclusively unidirectional. Data flows from the device to the care team and to coding for billing purposes. Interaction happens through other disconnected channels and is based solely on the existence of device readings. An out-of-range reading will trigger an alert-based interaction, but there is no context to the reading and the interaction is by its nature reactive. Remote care includes integrated communication channels. Platforms should facilitate proactive interaction efficiently and effectively, not just for the purpose of time tracking and CPT code submission.
- Remote care platforms should incorporate health disparity information, personal barriers, and individual motivations in a goal-based structure. Just knowing and establishing device reading parameters is insufficient. Remote care and monitoring platforms should capture personal patient environmental and motivational variables and facilitate goal setting between the two parties. Then they should bring this critical data (outside of just device readings) directly into the care team workflow.
- Finally, based on these, we should be measuring patient health outcomes tied to healthy behaviors, the reduction of risk and chronicity, health goal attainment, as well as device reading parameters. Yes, today we can avoid hospitalizations and readmissions by over 60%, which is a great start, but also not enough. We need to focus on how we are changing the health trajectory of patients.
Andrew Richburg-CEO
Technology Value-Based Care Providers Need, Part 3: “End-to-end technology experience that drives great outcomes at a reasonable cost”
This week we wrap up our series (read the other posts here!) unpacking a quote from an article in Patient Safety & Quality Healthcare where David Snow the chairman and CEO of Cedar Gate Technologies summarizes the technology and information gaps for value-based care providers saying, “Value-based care is an area full of innovation. The organizations that can create a high-value stack of analytics, with a meaningful high-touch consumer experience and end-to-end technology experience that drives great outcomes at a reasonable cost, will be the game-changers.”
Topics: health tech, healthcare technology, value-based care
Technology Value-Based Care Providers Need, Part 2: “Meaningful, high-touch patient experience”
This week we continue to unpack a quote from an article in Patient Safety & Quality Healthcare where David Snow the chairman and CEO of Cedar Gate Technologies summarizes the technology and information gap for value-based care providers saying, “Value-based care is an area full of innovation. The organizations that can create a high-value stack of analytics, with a meaningful high-touch consumer experience and end-to-end technology experience that drives great outcomes at a reasonable cost, will be the game-changers.”
Topics: healthcare technology, patient engagement
Technology Value-Based Care Providers Need, Part 1: “High-value Stack of Analytics”
Last week, we introduced an article from Patient Safety & Quality Healthcare that explains why the adoption of value-based healthcare has been accelerated by the pandemic, and why existing technology solutions aren’t meeting the needs of value-based providers. In the article, David Snow the chairman and CEO of Cedar Gate Technologies summarizes the technology and information gap we’re referring to saying, “Value-based care is an area full of innovation. The organizations that can create a high-value stack of analytics, with a meaningful high-touch consumer experience and end-to-end technology experience that drives great outcomes at a reasonable cost, will be the game-changers.”
Topics: healthcare technology, value-based care
Health Tech Spotlight podcast featuring our own, Andrew Richburg!
Health Tech Spotlight podcast featured our CEO & founder Andrew Richburg! Andrew talks about C3LX origins, our mission, his passions, and, of course, his dog Schmoopie! Take a listen:
Topics: healthcare technology
The adoption of value-based healthcare is accelerating across the country as the COVID-19 pandemic continues to bring to light many of the barriers to providing quality patient care in the existing fee-for-service and episodic sick care model. In Patient Safety & Quality Healthcare, the writer Matt Phillion explains why providers are making the shift and what tools they need to be successful in delivering quality, value-based care.
Topics: COVID, value-based care
As a global digital health company, we are excited to join StartUp Health on their mission to improve the health and wellbeing of everyone in the world. They open doors and increase our voice to health systems, partners, and investors. It is a critical time for us, and with StartUp, we could not be more thrilled about our future. StartUp Health recently introduced us to their community, by featuring C3LX in their newsletter explaining why they chose to invest in our mission.
Topics: healthcare technology, transforming healthcare, value-based care
C3LX Inc partners with athenahealth’s Marketplace Program to help value-based and Direct Primary Care practices remotely monitor patients, increase patient engagement, and achieve superior outcomes.
Topics: healthcare technology, transforming healthcare, value-based care
Recently, we’ve been sharing our vision for a technology platform that transforms the EHR beyond merely a digital documentation tool into a platform that empowers patients and clinicians towards improving health; both at an individual level and across a population. In order to achieve this vision, what are the key attributes and elements of this new comprehensive platform? Below is a summary of how we, at C3LX, are reimagining healthcare technology:
Topics: healthcare technology, transforming healthcare, value-based care