Care managers who support patient populations and other providers are critical for successful value-based models. Typically care managers are either a part of a diverse care team within an individual practice or they function as a centralized unit providing wrap-around support for patient populations spanning multiple practices. Unlike the workflow of the physicians within a practice that tend to focus on the patient in front of them or the schedule for the day, care managers can take a more proactive view looking ahead at patients that require more active attention and dynamic engagement.
Digital Health Capabilities to Effectively Support Value-Based Care: Tools for Care Managers
Topics: healthcare technology, transforming healthcare, value-based care
Digital Health Capabilities to Effectively Support Value-Based Care
Topics: COVID, health tech, healthcare technology, value-based care, telehealth
Digital Engagement is Here to Stay - Embracing Patient-Centric Technology
The use of telehealth rapidly increased during the spring as it gave patients a needed way to connect with their physician and reimbursement restrictions were lifted. During this time of a rapid increase in adoption, patients as consumers expect more from their digital tools and compare their experiences to offerings from other industries. Notably, as we head into fall, already the usage of telehealth offerings is declining as physician practices open back up and patients feel safer to return to in-person visits.
Topics: healthcare technology, transforming healthcare, patient engagement, telehealth
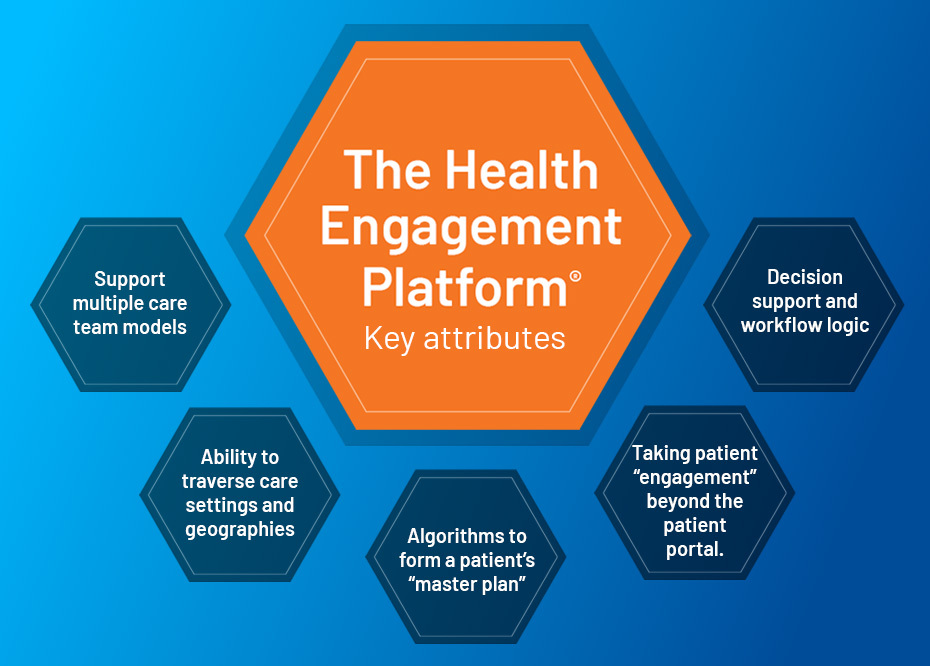
- Scheduling appointments, refilling prescriptions and looking up lab results are important, but true engagement comes first in understanding unique patient needs, wants, motivations and barriers to achieving care goals and the lifestyle changes needed to be successful; and then in supporting patients along the journey to achieving those goals.
- Patients rarely have just one, clear, manageable issue. A smart platform would take in a variety of inputs and combine appropriate algorithms for treating a patient’s asthma, arthritis, depression, and weight reduction without the clinician having to synthesize these disparate data points on their own.
- Each care team member is able to see both the patient’s master plan and the relevant data and prioritization that is specific to their role and scope of practice. With the growing dynamic of team-based care, each member has a personalized dynamic dashboard to work in.
- The master plan and supportive tools need to travel seamlessly with the patient, whether they are at home with devices tracking their activity, sleep, and blood pressure; or on the road for work or play, even when seeing a specialist. The primary care team then needs the relevant data and information to come back to them through the platform in meaningful and actionable ways.
- The platform must remind care team members and patients of upcoming and overdue activities, suggest changes in the master plan when patient conditions and care needs change, and route messages to the appropriate care team member regarding new test results, data trends negatively, or when patient health goals aren’t on track or being met. All of these long before an adverse event occurs.
At scale, the Health Engagement Platform facilitates the thousands of master plans seamlessly, undergirds a myriad of patient/provider workflows, simultaneously traverses multiple care settings, and supports hundreds of thousands of highly personalized provider decisions; so that a population can be proactively managed as never before. This is the future of healthcare technology!
Topics: healthcare technology, transforming healthcare, patient engagement
Patients hardly ever have just one clear, manageable issue. Even more importantly, people are multi-faceted, complex, and cannot be broken down to the presence or absence of a chronic condition. The Health Engagement Platform allows care teams to work with their patients to create a master plan that addresses all facets of their health journey; from treating a patient's asthma, arthritis, depression and weight reduction, while also understanding the intrinsic motivations and potential barriers affecting the necessary behavioral changes.
Topics: healthcare technology, transforming healthcare, patient engagement
“Our world is facing two pandemics right now. The acute one, Covid-19, is swift and relentless – and it’s disproportionately preying upon people affected by an even larger, more enduring pandemic: obesity.” Dr Rami Bailony
Topics: COVID, healthcare technology, transforming healthcare
How to Use Big Data Analytics to Increase Patient Engagement
Topics: healthcare technology, transforming healthcare, patient engagement
How To Meet the Needs of Non-Covid Patients During the Pandemic
Amidst today’s pandemic, health systems need to come up with a plan to approach non-Covid, or “non-urgent” patients, as their underlying health conditions are not going away, and in some cases, are worsening. At the beginning of the pandemic panic, these patients did not get the healthcare and support they needed, which has ultimately driven them to need additional care and put more strain on hospitals and care teams. In order to improve care and the systems in place currently, there are a couple steps health systems should take. One is innovating outpatient management to reduce demand at downstream bottlenecks, and the second is to utilize telehealth tools. Patients and physicians alike can benefit from this technology as it creates less exposure for both parties, and physicians can monitor the patient behavior and progress without having to rely on the patients to reach out when they are feeling especially ill.
Unfortunately, as more patients and health care providers lean further into telemedicine amid the pandemic, many are finding that while visits are moving into the future, health records are largely stuck in the past. There are good remote monitoring devices out there and if physicians can monitor their patient’s symptoms remotely, they can proactively handle their care and support; however, the patient generated health data coming to the physician must be actionable, meaningful and aggregated in such a way that it identifies patients needing further attention.
Check out how our Patient Engagement platform accomplishes this and learn more in this Harvard Business Review article.
Topics: healthcare technology, transforming healthcare, primary care
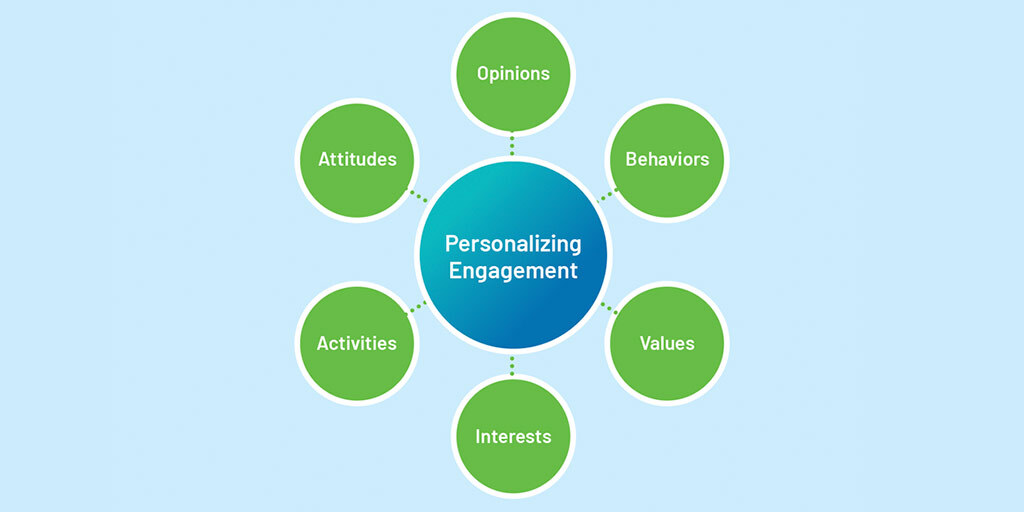
Not all patients are the same. Not all patients are unique.
At C3LX, we are passionate about personalizing healthcare by empowering patients. Through the use of technology, a deep understanding of patient types, & design thinking, we connect & reconnect patients and care teams in meaningful ways.
Topics: direct primary care, healthcare technology, transforming healthcare
YOU ARE THE DISRUPTOR. WE ARE THE ENABLER. THE C3LX PLATFORM FACILITATES THE CONNECTION BETWEEN YOUR PATIENTS AND YOU, THEIR TRUSTED CARE TEAM, REGARDLESS OF THE SETTING.
Topics: direct primary care, healthcare technology, transforming healthcare